Pathophysiology of the Nervous System: Cell Types and Pathologic Responses
Slides about Pathophysiology of the Nervous System. The Pdf, a Biology university presentation, explores cell types in the CNS, histological staining techniques, and astrocytic pathological responses, including astrogliosis and glial scar formation, with images and diagrams.
See more24 Pages

Unlock the full PDF for free
Sign up to get full access to the document and start transforming it with AI.
Preview
Cell Types in the CNS
Neurons -> the functional unit of the nervous system, they are excitatory cells that fire upon an action potential, there are many types Microglia Astrocyte Oligodendrocyte Neuron Glia -> includes astrocytes (provide homeostatic support to the neurons and plays an important role in regeneration), oligodendrocytes (myelin synthesis) and microglia (immune cell type important in inflammation , resident) Ependymal cells -> they are lining in the ventricle and provide homeostasis of the fluid inside, the CSF (cerebrospinal fluid).
In a pathological state (disease) there are conformational and molecular transitional changes such as degenerating neurons and an activation of the glia as a result of it.
Commonly Used Stains in Neuropathology
Haematoxylin and Eosin (H&E)
. Haematoxylin: is a basic dye (stains basophilic structures such as DNA and RNA that are negatively charged) stains nuclei blue/purple. It is not cell type-specific since it stains all the nuclei. Here we can see all the nuclei stained with hematoxylin: . Eosin: stains the cytoplasm (because it is an eosinophilic die) and the cell processes pink.
Both of these stains help us identify pathological features.
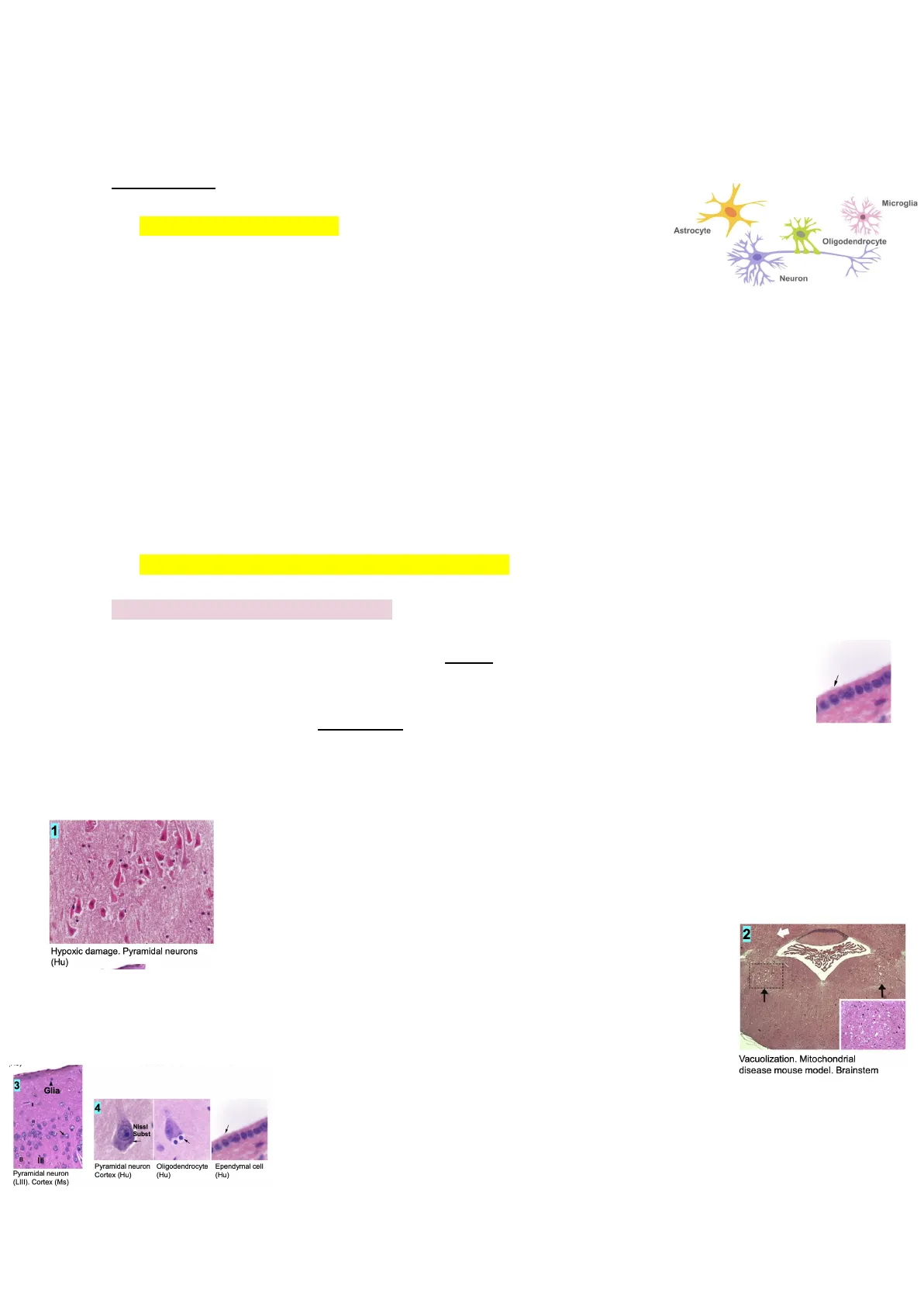
1 Hypoxic damage. Pyramidal neurons (Hu)
For example in degenerating neurons. The hypoxic damage can be caused by an isquemia (a lack of oxygen in the tissue). In this image we can see that all the cells are more bright pink (meaning this neurons are dying) called "red cells" which is a typical feature of hypoxic damage. These are pyramidal neurons in a human section.
We can also use them to identify vacuolization which are these holes in the middle of the tissue that cause loss of parenquima. So we can use hematoxylin and eosin to stain the parenquima and visualize the holes that are left after extensive vacuolization
2 Vacuolization. Mitochondrial disease mouse model. Brainstem
3 Glia
4 Nissl Subst Pyramidal neuron (LIII). Cortex (Ms)
Pyramidal neuron Oligodendrocyte Cortex (Hu) (Hu) Ependymal cell (Hu)
Finally we can use this stain to identify cell types. It is not super specific but since you are staining both the soma and nuclei it can provide you an idea of which is the cell type you are looking at. Visualized using light microscopy.
Luxol Fast Blue (LFB)
Is another tinctorial stain used to stain myelin in blue and is very useful to identify demyelinating lesions (when we have lesions that cause the loss of myelin we can no longer stain it with LFB).
This is important in different diseases such as multiple sclerosis in which there is an autoimmune reaction to myelin (there is a loss of myelin). EAE stands for experimental autoimmune encephalomyelitis is an experimental model of multiple sclerosis which process consists in the immunization of mice, injecting a protein of the myelin to them and different compounds to boost the immune response. So in both multiple sclerosis and EAE we can see demyelinating lesions.
Mi-WT B Ci-WT D Lesions LFB. Spinal cord (Ms). Ci: control-immunized, MOG-immunized A Ci-WT C Mi-WT Immune cells H&E. Spinal cord (Ms). Ci: control-immunized, Mi: MOG-immunized
B- This would we a control section (a control animal without EAE, so not immunized) C - This would be a mock immunized animal (animal with induced multiple sclerosis, EAE). We can see that the animal who has undergone this procedure has a lack of staining from the LFB.
We can combine the LFB with H&E in adjacent sections. Meaning we have for example the first section stained with LFB and the next section with H&E. In IMAGE C you can see that there are plenty of nuclei in the focal lesion area which correspond to immune cells destroying the myelin.
Visualized using light microscopy.
Congo Red (CR)
It is typically used to stain specifically amyloid deposits (which are red). We can see these in trauma, as senile plaques in Alzheimer's disease.
Control AD brain CR: Brain (Hu)
We can see a picture of a control brain (healthy human individual) compared with a section of a brain with AD in which all these -amyloid plaques can be identified with the CR stain.
This process follows the next steps: 1. Remove the brian. 2. Fixed to preserve the tissue and its proteins. 3. Section the tissue. 4. Passed onto glass slides. 5. Perform staining.
Instead of using human brains (Hu) we can also use CR to stain mouse models like these:
Control AD mouse models a b C d CR&H: Brain (Ms)
We can see that these models also develop this B-amyloid plaques. Visualized using light microscopy.
Thioflavin S
This is visualized using a fluorescence microscope (so its a fluorescence stain). Thioflavin S also binds to senil plaques (SP -> extracellular) but also to the neurofibrillary tangles (NFT -> intracellular) which are the two hallmarks of Alzheimer's disease (AD).
SPS LPS LPS SP> NFT> NFT> SP3 Alzheimer's disease brain (hippocampus; Hu) SP: senile plaque NFT: neurofibrillary tangles LP: Lipofuscin (autofluorescence)
It is a non-specific staining meaning these two structures (SP and NFT) are made up by different proteins (mostly B-amyloid and Tau respectively).
With Thioflavin S we can visualize a pigment called Lipofuscin (round shaped, they cannot be confused with SP nor NFT) which is especially abundant in diseased brains and mature brains (really old people's brains). The fact that we can ses LP confirms that this stain is non-specific.
Immunohistochemical Analysis
With these techniques we are using antibodies to detect specific antigens within the cell. These antibodies are normally comercial. Ex: if we want to identify an astrocyte we're going to buy an anti-GAFP antibody.
The difference between immunohistochemistry (IHC) and immunofluorescence (IF) is the detection method. In IHC we have a color product that we visualize with light microscopy and in IF we use the same procedure but visualize the signal using a fluorescence microscopy insead.
In both of them we have our tissue of interest that have different antigens such as GAFPs (marker for astrocytes), CK (marker for another cell type), ...
a) The first step is to incubate overnight with a primary antibody which is the one that recognizes the antigen (Ex: if we're detecting GFAP we use anti-GAFP antibodies as a primary antibody). b) Then we rinse the tissue using a wash buffer to remove all the primary antibody that has not bound to the tissue. c) We incubate with the secondary antibody which is for detection, and depending on our detecting method our secondary antibodies will be conjugated to an enzyme (IHC) or a fluorophore (IF). The secondary will recognize the primary due to its species meaning for example if the primary antibody is raised in goat the secondary antibody must be anti-goat -> so the secondary antibodies are non-specific (they will bind to all the primary antibodies raised in goat). To sum up we will buy a GAFP primary antibody that has been raised in goat and we will use a secondary that recognizes goat antibodies, therefore it will bind to the primary. -> The primary antibody is specific to the antigen. -> The secondary antibody is only for detection.
Immunohistochemistry (IHC) Immunofluorescence (IF) Coloured reaction product Signal DAB Peroxidase Light Fluorescant tag Secondary antibody Primary antibody Antigen of interest eg. GFAP, CK, EMA. Cell or tissue Cell or tissue
In IF we can do direct detection (we have a primary antibody conjugated to a fluorophore) or we can have a secondary antibody conjugated to a fluorophore. What is the difference? If we have secondary antibodies, we'll have multiple of them bind to a single primary antibody resulting in an amplified signal.
In IF, in contrast with IHC, we can perform a double labeling, meaning we can use different fluorophores and it can be in the same part of the cell.
-> In IHC once we do the reaction of the enzyme we'll have a precipitate which will be on top of the antigens. This means there will be no opportunity for other antibodies to bind to the tissue, because there is all this precipitate preventing the primary antibodies from binding to the tissue's antigens. -> In IF there is no precipitate, it's just a fluorophore emitting light when excited. Therefore, we could be recognizing an antigen with one primary antibody and the antigen next to it with another primary antibody raised in different species. If we want to co-localize to see if a specific protein is present in a specific cell type with double labelling to see if they are actually in the same place.
Astrocytes and Immunohistochemical Analysis
. When we do immunohistochemical analysis, for example for astrocytes, we typically use GFAP1. (with IHC or IF) . This protein is expressed at a basal level but it is also strongly expressed when they get really reactive and neoplastic, they change the morphology and they start expressing a lot of GFAP meaning it's a really good marker to identify reactive astrocytes (who are responding to damage). . We can use GFAP to identify Bergmann Glia which is a type of modified astrocytes in the cerebellum. . We can also use this to identify where to place electrodes, canulas, ... since we are going to do damage to the tissue and then we will see all these astrocytes reacting surrounding the cannula. - > this basically means that when we put a cannula and damage astrocytes, the amount of reaction of astrocytes gives us feedback about how much tissue damage we caused so we know we have to better our technique or even to know if we have reached the place we intended to. The amount of astrocytes reactive over time can also help us know if the cannula is being tolerated or not.
Image A - IHC
This is a double immunohistochemistry, and that is possible since the signal is in different places. In black we can see p-STAT3 in the nuclei G and GFAP is in the soma and processes. Since they are in different places, when we do the reaction with GFAP, we will have the precipitate all over the cell except in the nuclei and then the nuclei will perform the staining with p-STAT3 which is a transcription factor that responds to inflammation and then we can identify this. In this case, we use this method to see which are the astrocytes responding to inflammation. So p-STAT3 is a marker for when the cells respond to inflammation.
Double IHC GFAP/p-STAT3 (DAB+Nickel; NovaRed). Cerebellum (Ms). Inflammation mouse model (IL-6)
Meaning these cells are sensing some inflammation in the area, and that is why they are expressing/phosphorylating p-STAT3 so they are responding to this immune environment and we can see that the cells responding are astrocytes because they are stained by GFAP.
1 Stands for Glial Fibrillary Acidic Protein