Immunologia: sistema immunitario, immunità innata e adattativa
Documento sull'immunologia, il sistema immunitario, immunità innata e adattativa. Il Pdf, utile per lo studio universitario di Biologia, approfondisce argomenti come i trapianti, la tolleranza immunitaria, l'immunologia dei tumori e le malattie autoimmuni, con schemi e testo esplicativo.
Mostra di più23 pagine

Visualizza gratis il Pdf completo
Registrati per accedere all’intero documento e trasformarlo con l’AI.
Anteprima
IMMUNOLOGIA
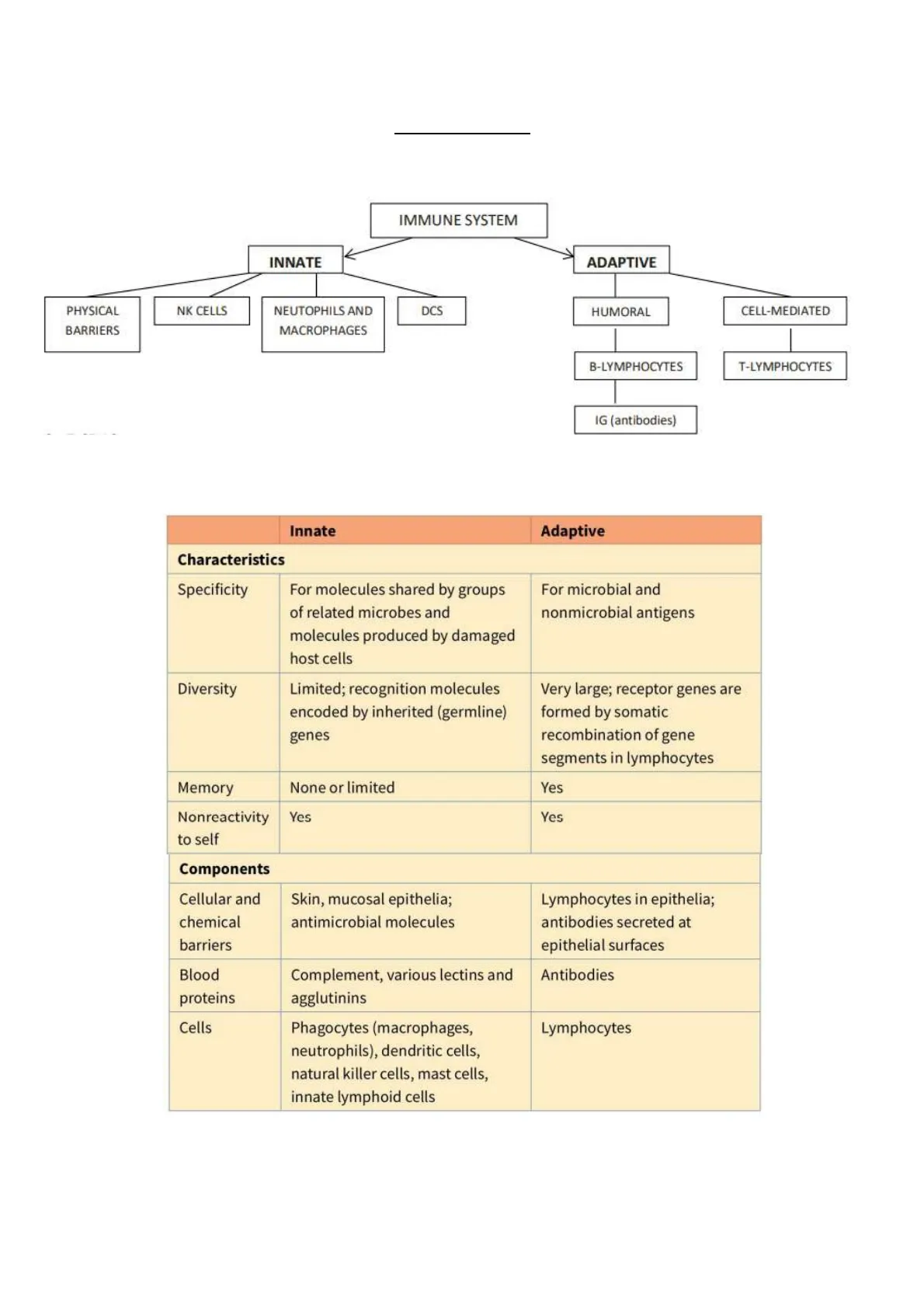
SCHEMA GENERALE DEL SISTEMA IMMUNITARIO
IMMUNE SYSTEM
- INNATE
- ADAPTIVE
PHYSICAL
BARRIERS
NK CELLS
NEUTOPHILS AND
MACROPHAGES
DCS
HUMORAL
CELL-MEDIATED
B-LYMPHOCYTES
T-LYMPHOCYTES
IG (antibodies)
Innate
Adaptive
Characteristics
Specificity
For molecules shared by groups
of related microbes and
molecules produced by damaged
host cells
For microbial and
nonmicrobial antigens
Diversity
Limited; recognition molecules
encoded by inherited (germline)
genes
Very large; receptor genes are
formed by somatic
recombination of gene
segments in lymphocytes
Memory
None or limited
Yes
Nonreactivity
to self
Yes
Yes
Components
Cellular and
chemical
barriers
Skin, mucosal epithelia;
antimicrobial molecules
Lymphocytes in epithelia;
antibodies secreted at
epithelial surfaces
Blood
proteins
Complement, various lectins and
agglutinins
Antibodies
Cells
Phagocytes (macrophages,
neutrophils), dendritic cells,
natural killer cells, mast cells,
innate lymphoid cells
Lymphocytes
RISPOSTA IMMUNITARIA INNATA E ADATTATIVA
Protective immunity against microbes is mediated by the early reactions of innate immunity
and the later responses of adaptive immunity.
Innate immune responses are stimulated by molecular structures shared by groups of microbes and by
molecules expressed by damaged host cells.
Adaptive immunity is specific for different microbial and nonmicrobial antigens and is increased by
repeated exposures to antigen (immunologic memory).
Many features of adaptive immunity are of fundamental importance for its normal functions.
These include specificity for different antigens, a diverse repertoire capable of recognizing a wide variety of
antigens, memory of antigen exposure, and the ability to discriminate between foreign antigens and self
antigens.
Immunity may be acquired by a:
- response to antigen (active immunity) or
- transfer of antibodies or effector cells (passive immunity).
LYMPHOCYTES are the only cells capable of specifically recognizing antigens and are thus the principal cells
of adaptive immunity. The total population of lymphocytes consists of many clones, each with a unique
antigen receptor and specificity.
The 2 major subsets of lymphocytes are B cells and T cells, and they differ in their antigen receptors and
functions.
The adaptive immune response is initiated by the recognition of foreign antigens by specific lymphocytes.
Specialized Antigen Presenting Cells (see chapter 7) capture microbial antigens and display these antigens
for recognition by lymphocytes-> Lymphocytes respond by proliferating and by differentiating into:
- effector cells, whose function is to eliminate the antigen, and into
- memory cells, which show enhanced responses on subsequent encounters with the antigen. The
elimination of antigens often requires the participation of various effector cells.
Humoral immunity is mediated by antibodies secreted by B lymphocytes and is the mechanism of defense
against extracellular microbes. Antibodies neutralize the infectivity of microbes and promote the
elimination of microbes by phagocytes and by activation of the complement system.
Cell-mediated immunity is mediated by T lymphocytes and their products, such as cytokines, and is
important for defense against intracellular microbes. CD4+ helper T lymphocytes help macrophages to
eliminate ingested microbes and help B cells to produce antibodies. CD8+ CTLs kill cells harboring
intracellular pathogens, thus eliminating reservoirs of infection.
So, the cardinal features of the adaptive immunity are:
- SPECIFICITY AND DIVERSITY: immune responses are specific for distinct antigens, and often for different
portions of a single complex protein. The part of the complex that is recognized by the lymphocyte is called
epitope or determinants. This antigenic specificity is possible thanks to the lymphocytes repertoire. And
this ability of the lymphocyte repertoire to recognize a large number of antigen is called diversity.
- MEMORY: exposure to a foreign antigen, enhances its ability to respond again to that antigen. This is why
the second immune response is usually stronger.
- CLONAL SELECTION: clones of lymphocytes are present in unimmunized individuals, and are able to
respond to foreign antigens.
- SELF TOLERANCE: is the immunologic unresponsiveness, called tolerance, with respect to self antigens.
Abnormalities in self tolerance can lead to autoimmune diseases.
PANORAMICA DELLE CELLULE DEL SISTEMA IMMUNITARIO
The anatomic organization of the cells and tissues of the immune system allows the rapid delivery of innate
immune cells, including neutrophils and monocytes, to sites of infection and allows a small number of
lymphocytes, specific for any antigen, to locate and respond effectively regardless of where in the body the
antigen is introduced.
The cells that perform the majority of effector functions of innate and adaptive immunity are PHAGOCYTES
(neutrophils and macrophages), MAST CELLS, BASOPHILS, EOSINOPHILS, DCS, and LYMPHOCYTES.
Cell
% counted
Relative #
Absolute #
ABS
Neutrophil
55-70
2500-8000
Lymphocyte
20-40
1000-4000
Monocyte
2-8
100-700
Eosinophil
1-4
50-500
Basophil
0-2
25-100
NEUTROPHILS-> the most abundant blood leukocyte with a distinctive multilobed segmented nucleus and
abundant cytoplasmic lysosomal granules, are rapidly recruited to sites of infection and tissue injury, where
they perform phagocytic functions.
MACROPHAGES-> include tissue resident sentinel cells, as well as cells derived from circulating monocytes
recruited in response to infection. All macrophages are phagocytic cells that ingest and kill microbes and
dead host cells and secrete cytokines and chemokines that promote the recruitment of leukocytes from the
blood and initiate the repair of damaged tissues (BETTER EXPLAINED CHAPTER 8.2)
DENDRITIC CELLS-> are cells with multiple extended cytoplasmic process, which are present in most tissues
of the body and function as innate sentinel cells and as APCs uniquely capable of activating naive T
lymphocytes (BETTER EXPLAINED CHPATER 8.1)
B AND T LYMPHOCYTES-> express highly diverse and specific antigen receptors and are the cells
responsible for the specificity and memory of adaptive immune responses (BETTER EXPLAINED CHAPTER 2,
3, 4, 5, 6)
INNATE LYMPHOID CELLS (ILCs)-> are cytokine-producing cells of the innate immune system with a
lymphocyte-like morphology. They perform similar functions to CD4+ or CD8+ effector T cells. ILCs, which
include NK cells, do not express highly diverse, clonally distributed antigen receptors.
Both B and T lymphocytes arise from a common precursor in the bone marrow. B cell development
proceeds in the bone marrow, whereas T cell precursors migrate to and mature in the thymus. After
maturing, B and T cells leave the bone marrow or thymus (respectively B-> bone marrow, T->thymus),
enter the circulation, and populate peripheral lymphoid organs.
Naive B and T cells are mature lymphocytes that have not been previously stimulated by antigen.
When they encounter antigen, they proliferate and differentiate into effector lymphocytes that have
functions in protective immune responses. Effector B lymphocytes are antibody-secreting plasma cells.
Effector T cells include cytokine-secreting CD4+ helper T cells and CD8+ Cytotoxic T-Lymphocytes.
Some of the progeny of antigen-activated B and T lymphocytes differentiate into memory cells that survive
for long periods in a quiescent state. These memory cells are responsible for the rapid and enhanced
responses to subsequent exposures to antigen.
TESSUTI DEL SISTEMA IMMUNITARIO
The organs of the immune system may be divided into the primary
lymphoid organs (bone marrow and thymus), where lymphocytes
mature, and the peripheral, or secondary, organs (lymph nodes,
spleen, and parts of the mucosal immune systems), where naive
lymphocytes are activated by antigens.
Bone marrow contains the stem cells for all blood cells, including
lymphocytes, and is the site of maturation of all of these cell types
except T cells, which mature in the thymus.
Extracellular fluid (lymph) is constantly drained from tissues
through lymphatics into lymph nodes and eventually into the blood.
Microbial antigens are carried in soluble form and within DCs in the
lymph to lymph nodes, where they are recognized by lymphocytes.
Immune System
Mucous
Membranes
Tonsils
Lymphatic
Vessels
Thymus
Lymph
Nodes
Skin
Spleen
Bone
Marrow
Lymphatic
Vessels
LYMPH NODES are encapsulated secondary lymphoid organs located throughout the body along
lymphatics, where naive B and T cells respond to antigens that are collected by the lymph from peripheral
tissues. The spleen is an encapsulated organ in the abdominal cavity where senescent or opsonized blood
cells are removed from the circulation, and in which lymphocytes respond to blood-borne antigens.
Lymph nodes and the white pulp
of the spleen are organized into
B cell zones (the follicles) and I
cell zones. The T cell areas are
also the sites of residence of
mature Dendritic Cells, which
are Antigen Presenting Cells
specialized for the activation of
naive T cells.
A lymph node
secondary
primary
lymphoid follicle
(mostly B cells)
lymphoid follicle
(with germinal center)
medullary cords
(macrophages
and plasma cells)
afferent
lymphatic vessel
medullary sinus
artery
vein
paracortical area
(mostly T cells)
efferent
lymphatic vessel
senescent
germinal center
germinal center
marginal sinus
MIGRAZIONE DEI LEUCOCITI NEI TESSUTI
Leukocyte migration from blood into tissues occurs through postcapillary venules and depends on
adhesion molecules expressed on the leukocytes and vascular endothelial cells as well as chemokines:
- SELECTINS are carbohydrate-binding adhesion molecules that mediate interaction of leukocytes with
endothelial cells (of the vessel), the first step in leukocyte migration from blood into tissues.
. E-selectin and P-selectin are expressed on activated endothelial cells and bind to selectin ligands on
leukocytes
. L-selectin is expressed on leukocytes and binds ligands on endothelial cells.
- INTEGRINS are a large family of adhesion molecules, some of which mediate tight adhesion of leukocytes
with activated endothelium, a critical step in leukocyte migration from blood into tissues. The important
leukocyte integrins include:
· LFA-1 which bind to ICAM-1
· VLA-4 which bind to VCAM-1, on endothelial cells.
- CHEMOKINES and other signals at sites of infection increase the affinity of integrins on leukocytes, and
various cytokines (TNF, IL-1) increase the expression of integrin ligands on endothelium. Chemokines are a
large family of cytokines that stimulate leukocytes movement and regulate migration. There are many
types:
o
CC CHEMOKINES-> made of 2 cysteine residues and induce the migration of monocytes, NK cells
and DCs.
o CXC CHEMOKINES-> 2 cysteine residues separated by an aminoacid. Only the CXC that contains the
ELR functional motifs, are able to control the neutrophils migration. The others act on monocytes
and other cells.
o C CHEMOKINES-> single cysteine residue.
o CX3C CHEMOKINE-> 2 cysteine separated by 3 amino acids.