Skin infections: viral, fungal, and parasitic types, by Prof. Stefania Guida
Slides from Prof. Stefania Guida about Skin Infections. The Pdf, a university-level Biology resource, details viral infections like Herpes Simplex, fungal infections such as Tinea Favosa, and parasitic conditions like Scabies, providing clear explanations and visual aids.
See more24 Pages

Unlock the full PDF for free
Sign up to get full access to the document and start transforming it with AI.
Preview
Rachele Follese Prof. Stefania Guida
Integumentary System, SG1
Skin Infections
Viral Infections Overview
In the picture on the right, examples of cutaneous viral infections can be seen. The most common types of infections are those caused by Herpes Simplex Viruses, Varicella Zoster Virus, Human Papilloma Virus and Molluscum Contagiosum. Other minor infections can however be seen.
Viral Infection - Skin Types
Viral infection - skin HERPES SIMPLEX HERPES ZOOSTER HSV 1 - HSV2 VZV WARTS PAPOVA VIRUS HUMAN PAPILLOMA VIRUS HPV 3 CONDYLOMATA ACUMINATA HPV 2 HPV 1 HPV 6 -11 16 -18 MOLLUSCUM CONTAGIOSUM POXVIRUS ORF PARAPOX VIRUS SIND. hand-feet-mouth COXSACKIE
If primary skin lesions had to be associated to specific viral infections manifestations, all the herpetic viral infections appear with grouped vesicles: this is a major clinical hint for diagnosis. Instead, HPV infection causes warts, that are mainly composed of papules.
Herpes Viruses
Herpes Viruses Characteristics
Herpes viruses are DNA viruses characterized by a high molecular weight. The most important aspect to consider when talking about infectious pathogens is the way in which the virus reaches and infects a person. In this case, there can be either cutaneous- mucosal or direct mucosal contacts, as the infections can happen both at the level of the skin and at the level of the mucosae.
Types of Herpetic Viruses
There are different types of herpetic viruses:
- HSV-1, mainly responsible for the classical herpetic lesions around the mouth and nose. The very first appearance of HSV-1 infection can arise with gingivitis or stomatitis, with the affection of the oral cavity.
Gingivitis-Stomatitis Symptoms
Gingivitis-stomatitis Located on the lips, gums, palate, cheeks; sparing the tongue and oropharynx Intense pain, drooling, halitosi, difficult to eat, lymphadenitis, fatigue, fever Polymorphic evolution Spontaneous healing in 7-10 days without any scars usually
- HSV-2, considered the herpetic virus for the genital area (so it is considered as a sexually transmitted disease). It is however important to note that there can be HSV-2 infection of the mouth, as well as HSV-1 infection of the genitalia depending on the route of transmission of the virus.
- HHV-3, also known as Varicella Zoster Virus. It causes chickenpox, mainly in children who did not receive the vaccination, and shingles (also known as Herpes Zoster).
- HHV-4, also known as Epstein-Barr Virus. It causes mononucleosis and immunoproliferative diseases (Burkitt lymphoma, nasopharyngeal carcinoma, oral leukoplakia).
- HHV-5, also known as Cytomegalovirus. It is responsible for primary infections of the salivary glands.
Page 1 of 24Rachele Follese Prof. Stefania Guida Integumentary System, SG1 28/02/2024
Herpetic Lesions Appearance
As previously stated, herpetic lesions usually appear as grouped vesicles, which when eroded lead to crust formation. Depending on the potential superinfection with bacteria, crusts may also leave scars. Otherwise, in case of no further complications, there will be no scar formation because these are very superficial lesions.
Herpes Simplex Viruses
Herpes Simplex Ubiquity and Endemic Nature
Herpes Simplex viruses are ubiquitous, and the infection is endemic:
- When talking about HSV-1, the infection is acquired through direct contact and sexual infection is not mandatory.
- HSV-2, instead, is considered as a sexually transmitted disease.
Incidence of HSV-1 and HSV-2
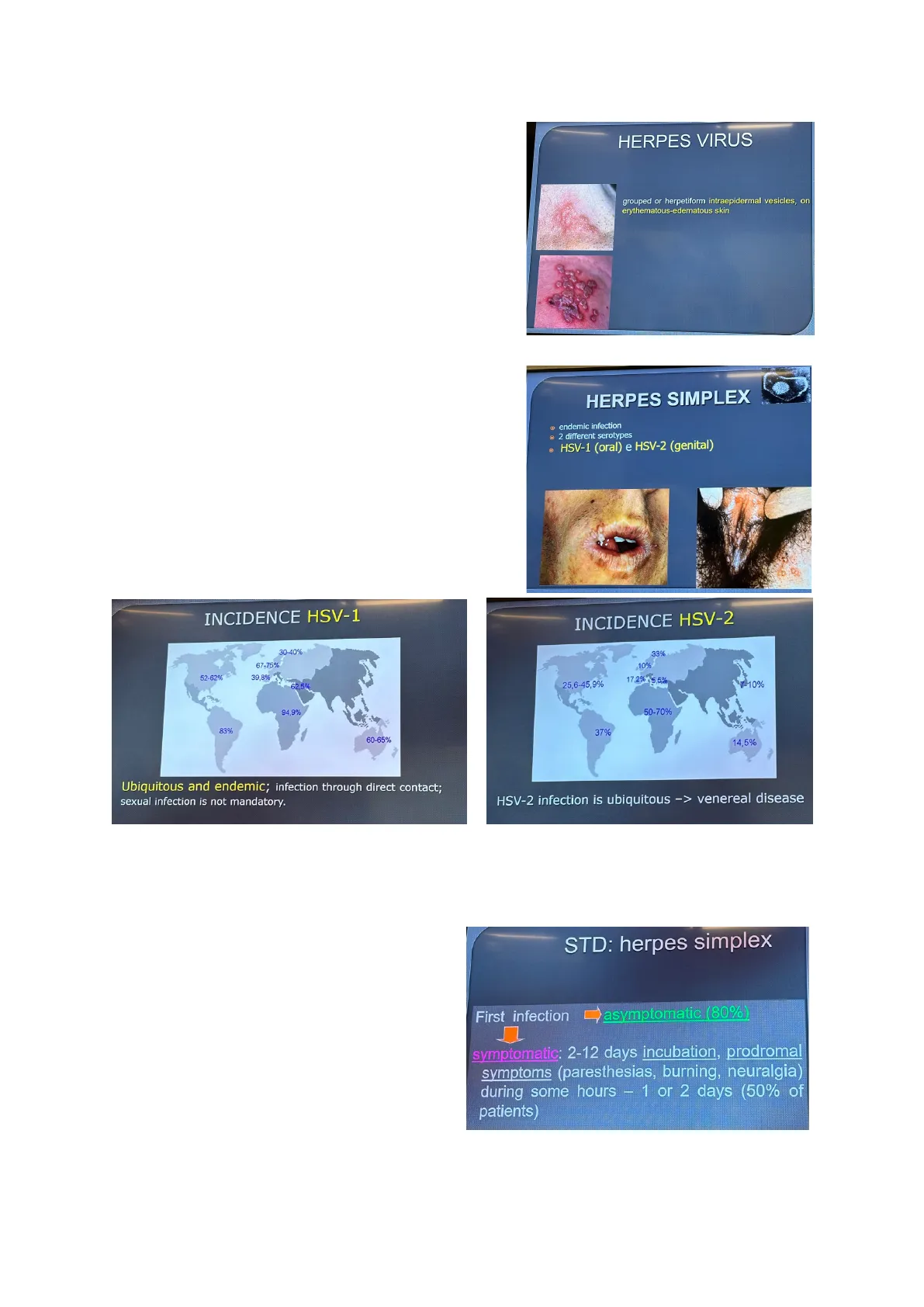
The pictures below depict the incidence of both viruses. INCIDENCE HSV-1 30-40% 67-75% 52-62% 3 39,8% 62,5% 94,9% 83% 60-65% Ubiquitous and endemic; infection through direct contact; sexual infection is not mandatory. HERPES VIRUS grouped or herpetiform intraepidermal vesicles, on erythematous-edematous skin HERPES SIMPLEX
- endemic infection
- 2 different serotypes
- HSV-1 (oral) e HSV-2 (genital)
INCIDENCE HSV-2 33% 10% 17,2% 5,5% 25,6-45,9% 7-10% 50-70% 37% 14,5% HSV-2 infection is ubiquitous -> venereal disease
Asymptomatic Infection and Latency
Something quite interesting about the herpes simplex infections is that many people have had contact with these viruses, even though not everyone developed the clinical symptoms of the infection (as a matter of fact, 80% of infected people are asymptomatic). However, even in these cases, there will be the typical latency period of the infection, in which the STD: herpes simplex virus reaches the sensitive ganglion, and, after that, people may experience recurrences due to viral reactivation. First infection asymptomatic (80%)
Viral Reactivation and Recurrences
So, in other words, it can happen that in adult life, there can be a potential reactivation of the virus even though the patient did not have a 1st manifestation at the time of infection. Recurrences mainly happen when the immune defenses do not work properly, with the virus reaching the skin. symptomatic: 2-12 days incubation, prodromal symptoms (paresthesias, burning, neuralgia) during some hours - 1 or 2 days (50% of patients)
Page 2 of 24Rachele Follese Prof. Stefania Guida Integumentary System, SG1 28/02/2024
First Infection vs. Recurrence Symptoms
Moreover, there are differences between 1st infections symptoms and recurrence symptoms. The lesions are pretty much the same, but, in the case of first infection, there is also the presence of systemic symptoms like fever, pain, lymph node involvement and inflammation. Instead, recurrences are characterized just by the presence of the lesion, which can be associated with a burning sensation usually felt before the clinical manifestation.
Herpes Labialis Recurrence
RECURRENCE: herpes labialis Limited skin lesions associated with prodromal burning sensation The surrounding skin can appear inflamed and with edema. Sometimes, there could be the presence of confluent vesicles, which is however quite atypical.
Factors Increasing Recurrence
Factors associated with increased recurrence are:
- Fever
- UV exposure
- Trauma
- Stress
- Alcohol
- Infectious disease
- Immunosuppressive drugs
- Immunodeficiency
Herpes Lesion Location
Despite what one might think, these lesions can be found anywhere in the body, depending on the area of contact. For example, a peculiar lesion, mostly found in people that directly handle the virus in labs, is the herpes gladiatorum, which is found on the fingers.
Herpes Gladiatorum
HERPES GLADIATORUM Professional disease
Page 3 of 24Rachele Follese Prof. Stefania Guida Integumentary System, SG1 28/02/2024
Genital Herpes Simplex
Genital Herpes Simplex Causes and Risk Factors
Genital herpes simplex infection, instead, is caused in 25% of cases by HSV-1 and in the remaining 75% by HSV-2. The risk of infection increases with:
- Age (17-28 years old); 20% of adults
- Numbers of age of sexual activity
- Number of sexual partners
First Genital Herpes Infection Symptoms
First infection Genital Herpes Simplex Symptoms: headache, sindrome simil influenzale, lymphadenitis, abdominal pain, fever, myalgias (40% first infection). Symptoms last 2 weeks, healing requires 10-12 days.
Healing Time for Genital Herpes
The first infection is characterized by systemic symptoms, which last at least 2 weeks. The complete healing of the lesions then needs another 2 weeks (so it takes one month in total). Instead, recurrences usually last 7-10 days (this is true both for the genital and cutaneous infections).
Eroded Lesions and Polycyclic Contours
Depending on the lesion, either the vesicles themselves or what the erosions left of them can be appreciated. Something that can give the suspicion of HSV infection is the fact that the eroded lesions have curved borders (polycyclic contours of the lesion), which could lead the dermatologist to think that previously, there were vesicles in that area of skin.
Extra Genital Localization of Infection
As one can imagine, there may also be a progression in the surrounding area as compared to the first manifestation of the herpetic lesions. In this case, extra genital localization of the infection can cause:
- Proctitis
- Pharyngitis
- Kerato-conjunctivitis
- Whitwit
Triggering Factors for Recurrent Genital Herpes
Again, recurrent genital herpetic lesions can be related to triggering factors, such as sexual intercourses, menstrual cycle, concomitant infections, stress, UV exposure and immunosuppression.
Page 4 of 24Rachele Follese Prof. Stefania Guida Integumentary System, SG1 28/02/2024
Congenital Herpes
Congenital Herpes Incidence and Transmission
Congenital herpes has an incidence of 1/10.000 cases and transmission can happen:
- During delivery (90%), if the lesions are located on the genitalia of the mother
- Through transplacental route (5%)
Mother with active herpes infection (although active infection may not be apparent) Blisters due to congenital herpes Diagnosis *ADAM.
Viral Shedding and Contagion
In some cases, it may happen that an individual does not show any specific lesion, however they can still be contagious due to viral shedding with no clinical appearance. This explains why these infections are so widespread.
HSV Infection Diagnosis
When we have the suspicion of HSV infection, but lesions are not clear cut, there are tests helping in the diagnosis. These tests are rarely used, as, usually, the diagnosis can be done based just on appearance of the lesions. Among all tests, the PCR test is the most used. Serology is not interesting because, just by knowing the positivity of IgG you cannot diagnose the infection. However, in case of suspected 1st infections, which cannot be easily diagnosed (for example due to bacterial superinfection that mask the clinical aspects of the infections), IgM positivity can help.
Other Diagnostic Aids
Other aids for diagnosis are:
- Culture
- Immunofluorescence
- Microscopy
Treatment
Antiviral Treatment for Herpes
These lesions are not usually treated with oral antiviral treatment. However, the topical antiviral cream (or gel) can be used if the patient has the burning sensation. Once the vesicles are out, the cream does not have any effect because the virus is already spreading. In this case an antibiotic cream on the crust is used to avoid superimposed bacterial infections. If a patient has many recurrences in a year or a painful or discomforting lesion on genitalia, oral antiviral can be used (can be taken up to months).
Interactions HIV-HSV
HIV-HSV Lesion Differences
When a patient has HIV, the lesions can appear in a very different way with respect to a non- HIV-infected person. As a matter of fact, due to the already disrupted immune system, lesions can be necrotic, with the consequent development of deeper erosions and overall different course of the disease.
Page 5 of 24Rachele Follese Prof. Stefania Guida Integumentary System, SG1 28/02/2024
HIV-HSV Interaction Diagram
INTERACTIONS HIV-HSV HSV in HIV Pz HIV negativo Pz HIV positivo HIV: HSV: SYMBIOSIS - Sexual risk behaviour
Varicella Zoster Virus
Varicella Zoster Virus Conditions
Varicella Zoster Virus infections give rise to two important conditions that are characterized by different clinical manifestations:
- Chickenpox, characterized by presence of vesicles (that sometimes evolve into pustules) that are centered by an area of depression. These lesions involve the whole body, including the scalp
- Shingles (or herpes zoster), in which lesions are formed by grouped vesicles, that tend to be unilateral and distributed along a dermatome1. 1-7 days before the eruption of the vesicles, prodromal symptoms including pain arise.
HHV3 - Varicella / Herpes Zoster
HHV3 - varicella / Herpes Zoster
Latency and Recurrence of VZV
The reason why the same virus can give rise to two different clinical conditions is because after the 1st infection (that gives rise to chickenpox), the virus undergoes a period of latency, in which it migrates into a ganglion. For this reason, in case of recurrence, the lesion will only manifest along the areas of distribution of the nerve (giving rise to shingles).
Grouped and Hemorrhagic Vesicles
Sometimes, when there are too many grouped vesicles, they tend to have an underlying erythema and they may seem to be confluent. In other cases, there may be some hemorrhagic vesicles because of the violence of the appearance .
1 Areas of the skin whose sensory distribution is innervated by the afferent nerve fibers from the dorsal root of a specific single spinal nerve ganglion.
Page 6 of 24 Immune system